Program-Specific Associate Professor (Chief) Akio Sakamoto
The purpose of our research program is the reconstruction of musculoskeletal disorders in orthopaedic surgery. The loss of locomotor function reduces the patient’s quality of life. if it takes time to reconstruct the function, there is a risk of disuse syndrome and complications of other organ diseases. Rapid functional reconstruction using artificial joint, metal implant, and artificial bone is desired for such patients. We are developing patient-specific and disease-specific medical device for next-generation surgery.
Research and Education
Artificial joint:
We are developing original artificial hip joint implant, which have superior mechanical properties and biocompatibility. Currently we are developing bioactive bone cements for arthroplasties, as well as bioabsorbable screws for the reconstructive surgeries. The artificial knee joint aims to improve long-term durability and patient satisfaction by analyzing the knee joint kinematics using computer simulations.
New designed metal plate:
We are developing new plates that can be used not only for bone fractures but also for tumor (primary and metastatic) surgery.
Spinal fusion cage:
We have developed a spinal fusion cage using bioactive porous titanium porous and are applying it clinically.
Biomaterials:
We are developing artificial bones that have a high affinity with living bone. By applying special treatment to the surface of titanium metal and polymer, we are developing new artificial bones and artificial joints that have functions such as bone formation and antibacterial properties. And additive manufacturing technology is introduced to realize the patient-specific and disease-specific devices.
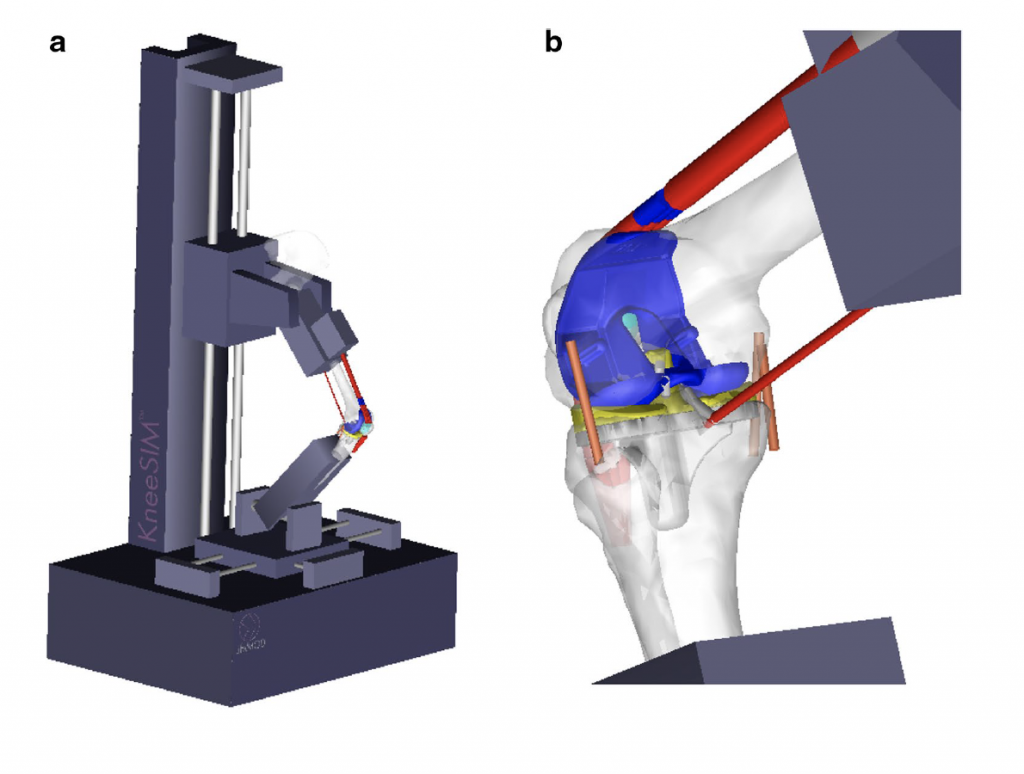 Figure1: Computer simulation of artificial knee joint
Figure1: Computer simulation of artificial knee joint
 Figure2: Clinical trial of spinal fusion using custom-made bioactive porous titanium device.
Figure2: Clinical trial of spinal fusion using custom-made bioactive porous titanium device.
https://www.kuhp.kyoto-u.ac.jp/press/20211210.html
Recent Publications
- Sakamoto A, Noguchi T, Matsuda S. Combined latissimus dorsi and scapular flaps for reconstruction of a large defect after a shoulder sarcoma resection. J Surg Case Rep. 2023 Mar 18;2023(3)
- Umeda K, Sakamoto A, Noguchi T, Uchihara Y, Kobushi H, Akazawa R, Ogata H, Saida S, Kato I, Hiramatsu H, Uto M, Mizowaki T, Haga H, Date H, Okamoto T, Watanabe K, Adachi S, Toguchida J, Matsuda S, Takita J. Clinical Outcomes of Patients With Osteosarcoma Experiencing Relapse or Progression: A Single-institute Experience. J Pediatr Hematol Oncol. 2023 Apr 1;45(3):e356-e362.
- Nakamura S, Tanaka Y, Kuriyama S, Nishitani K, Watanabe M, Yamauchi K, Song YD, Matsuda S. Anteromedial Tibial Attachment in Single-Bundle Anterior Cruciate Ligament Reconstruction Can Represent Normal Kinematics in Computer Simulation. J Knee Surg. 2023 Jun;36(7):731-737.
- Nakamura S, Kuriyama S, Ito H, Nishitani K, Song YD, Ikebe S, Higaki H, Matsuda S. Kinematic comparison between asymmetrical and symmetrical polyethylene inserts during deep knee bend activity. J Orthop Sci. 2022 Jul;27(4):810-814.
- Morita Y, Saito M., Rangel-Moreno J, Franchini A.M, Owen J.R, Martinez J.C, Daiss J.L, de Mesy Bentley K.L, Kates S.L, Schwarz E.M, Gowrishankar M. Systemic IL-27 administration prevents abscess formation and osteolysis via local neutrophil recruitment and activation. Bone Res. 2022 Aug 26;10(1):56.
Laboratory
Program-Specific Associate Professor (Chief):Akio Sakamoto
Program-Specific Associate Professor:Shinichiro Nakamura
Program-Specific Assistant Professor:Yugo Morita
